Oct 5, 2018 | Digital Pathology, Instruments & Equipment, Laboratory Management and Operations, Laboratory News, Laboratory Pathology, Laboratory Testing, Management & Operations
New dichromatic color scale developed by scientists at the Pacific Northwest National Laboratory could play a role in how slides are stained and how software color-codes digital pathology images in ways that make it easier for human eyes to recognize structures and features of interest
Clinical laboratories, anatomic pathologists, and other specialized diagnostics providers play an essential role in precision medicine. Imagine, however, performing surgical pathology analysis on slides using displays that cannot recreate—or worse, inaccurately display—a range of colors used in the image being analyzed.
As many as 8% of men and 0.5% of women of Northern European ancestry already experience issues discerning colors in the interfaces, information, and world around them due to red-green color blindness according to the National Eye Institute. This can lead to potential for misreadings and medical errors.
Now, research from Pacific Northwest National Laboratory (PNNL) holds the potential to establish a standard colormap that eliminates the impact of red-green colorblindness on visuals. Surgical pathologists, for example, spend much of their days viewing slides and/or digital pathology images. Thus, any new method of illustrating/coloring/highlighting features of interest could eventually prove to be a useful innovation in the specialty of anatomic pathology.
In completing their research, the PNNL scientists created an open-source tool called Cmaputil that other researchers can use. Could it enable clinicians and laboratory workers to improve the visibility of critical elements in samples, slides, and other visual data formats used daily at medical laboratories and anatomic pathology groups?
PLOS One published details about the development of the colormap and its potential scientific applications in August.
PNNL’s Cividis Color Scale: A Better Alternative to Rainbow Color Scales?
While the typical rainbow color map draws attention to a chart or image, it is not particularly great at conveying information—especially if the reader is color vision deficient (CVD) or color blind. Yet, despite this, rainbow scales are common in everything from local weather reports and news stories to medical images and medical studies.

Jamie Nuñez, lead author of the PLOS One study and a chemical and biological data analyst at PNNL, told Scientific American, “People like to use rainbow because it catches the eye. But once the eye actually gets there, and people are trying to figure out what’s actually going on inside of the image, that’s kind of where it falls apart.” (Photo copyright: University of Washington.)
PNNL scientists started with the viridis colormap due to “its wide range of colors” and “overall sharpness when overlaid with complex images.” They created an open-source software tool capable of taking existing color scales and simulating the visual effect of red-green color blindness using a mathematical model of human sight. Their software adjusts the scale so that color and brightness vary at a steady rate.
Their adaptions resulted in what they call the “cividis colormap.” It is a blue and yellow scale that provides an accurate change in hue and luminance when compared to changes in the data set. Researchers noted that, to their knowledge, this is the first study to mathematically optimize a colormap specifically for viewing by both those with CVD and those with normal vision.
“Here, we present an example CVD-optimized colormap created with this module that is optimized for viewing by those without a CVD as well as those with red-green colorblindness. This colormap, cividis, enables nearly-identical visual-data interpretation to both groups, is perceptually uniform in hue and brightness, and increases in brightness linearly,” the researchers noted in the PLOS One study.
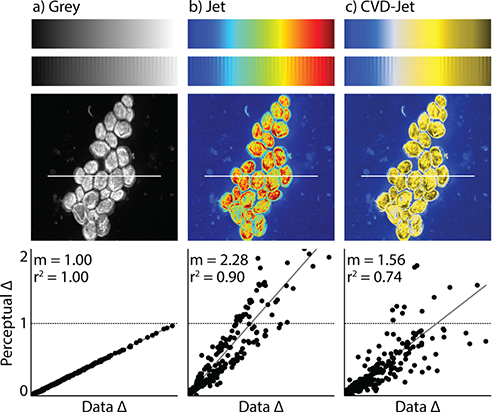
Example above is of a misleading colormap, taken from the PNNL/PLOS One study. An image of yeast cells is shown in gray scale (left), with a rainbow color scale (middle) and as a person with red-green color blindness sees the rainbow image (right). (Photo/caption copyright: Nuñez JR, Anderton CR, Renslow RS (2018) PLoS ONE 13(7): e0199239/Scientific American.)
The PNNL researchers report that the colormap will soon be ready in a number of tools, including:
According to Scientific American, cividis will be added to the color-scale libraries of roughly a dozen software packages.
“While it may take some time for the full scientific community to both be aware of the need to choose appropriate colormaps and agree on preferred colormaps,” PNNL researchers note, “we hope the code we provide here can help with this transition by allowing others to experiment with the different aspects of colormap design and see how the various characteristics of a colormap affect its interpretation.”
They are concerned that the changing color spaces on future displays may make current colormaps and standards obsolete, as they display colors outside the standard sRGB color space. However, the researchers also note that any change to color spaces could result in an increase in color availability and allow cmaputil to create better-optimized color schemes.
How Cividis and Similar Approaches Might Impact Pathology
While the technology was developed with mass spectrometry and fluid flow analysis in mind, it could prove useful for medical laboratories and specialized diagnostics providers as well—in particular, anatomic pathology and surgical pathology labs.
Coverage of a presentation at the 2011 IEEE Information Visualization Conference by Phys.org highlights a similar concept for diagnosing heart disease. By taking 3D representations of arteries using a rainbow colormap and converting them to 2D projections using a dichromatic black to red colormap, Harvard researchers found their HemoVis tool increased diagnostic accuracy from 39% to 91% in their study.
Technologies and techniques designed for scientific applications often find use in healthcare environments. For anatomic and surgical pathologist and other diagnostics providers, the research from PNNL shows promise for adapting the latest data visualization trends to further improve accuracy, efficiency, and accessibility of medical images, samples, and other complex images used daily in the process of diagnosing disease.
—Jon Stone
Related Information:
End of the Rainbow? New Map Scale Is More Readable by People Who Are Color Blind
Optimizing Colormaps with Consideration for Color Vision Deficiency to Enable Accurate Interpretation of Scientific Data
Evaluation of Artery Visualizations for Heart Disease Diagnosis
NanoSIMS for Biological Applications: Current Practices and Analyses
New Color Scale Makes Data Visualizations Easier for Colorblind People to Read
The End of the Rainbow? Color Schemes for Improved Data Graphics
Time to Replace ‘Rainbow Color Scale’ for Data Visualization?
How a New Color Scale for Scientific Models Could Improve Healthcare
To Diagnose Heart Disease, Visualization Experts Recommend a Simpler Approach
Oct 1, 2018 | Digital Pathology, Instruments & Equipment, Laboratory Instruments & Laboratory Equipment, Laboratory Management and Operations, Laboratory News, Laboratory Operations, Laboratory Pathology, Laboratory Testing, Management & Operations
New advancements in mHealth, though encroaching on testing traditionally performed at clinical laboratories, offer opportunity to expand testing to remote locations
Mobile technology continues to impact clinical laboratories and anatomic pathology groups and is a major driver in precision medicine, as Dark Daily has reported. Most of the mobile-test development which incorporates smartphones as the testing device, however, has been for chemistry and immunoassay types of lab tests. Now, a new developer in Monmouth Junction, NJ, has created a Complete Blood Count (CBC) test that runs on devices attached to smartphones.
Such devices enable doctors to order test panels for patients in remote locations that also may lack resources, such as electricity.
The developer is Essenlix and it calls its new testing device iMOST (instant Mobile Self-Testing). According to the company’s website, which is mostly “Under Construction,” iMOST can provide “accurate blood and other healthcare testing in less than 60 seconds by a smartphone and matchbox-size-attachment, anywhere, anytime, and affordable to everyone.”
The company description on the Longitude Prize website states that Essenlix “uses multidisciplinary approaches to develop a new innovative platform of simple, fast, ultrasensitive, bio/chemical sensing and imaging for life science, diagnostics, and personal health.
The Longitude Prize competition was established to promote the invention of “an affordable, accurate, fast and easy-to-use test for bacterial infections that will allow health professionals worldwide to administer the right antibiotics at the right time,” the website states.

The Essenlix iMOST mobile-testing device (above) connects to a smartphone (shown right) and enables clinical laboratory technicians to run tests in remote locations from samples taken at time the test. Though still in trials, iMOST, and other similar devices, promise to expand testing to outside of traditional medical laboratory locations and further promote precision medicine. (Photos copyright: Lydia Ramsey/Business Insider.)
Essenlix’s iMOST mobile testing system consists of:
- a mobile application (app);
- the device attachment, which goes over the phone’s camera; and,
- a cartridge that holds a sample of blood.
So far, there have been two trials with a total of 92 participants, comparing traditional CBC testing with the Essenlix test. The results were within the FDA’s requirements for allowable error, prompting Chou to tell Business Insider, “Our error is clearly smaller than the FDA’s requirement, so the data is very, very good.”
Chou and his team are working toward FDA approval.
Other Testing Devices That Attached to Smartphones
Aydogan Ozcan, PhD, Professor of Electrical Engineering and Bioengineering at UCLA, and Mats Nilsson, PhD, Professor and Scientific Director of the Science for Life Laboratory at Stockholm University, have developed an attachment that they say can transform “a phone into a biomolecular analysis and diagnostics microscope,” according to The Pathologist. Dark Daily has published many e-briefings on Ozcan’s innovations over the years.
Their goal, the researchers said, was to create technology that can be used in low- and middle-income areas (LMICs), as well as in more advanced locations, such as Sweden. “I’ve been involved in other projects where we’ve looked at point-of-care diagnostic approaches,” he said, “and it seems to be very important that the devices [do not] rely on wired electricity or networks to serve not only LMICs, but also modern, developed environments. It’s often difficult to find an available power socket in Swedish hospitals.”
The molecular diagnostic tests that can be done with smartphone attachments—such as those developed by Ozcan and Nilsson—represent another way of using a smartphone in the healthcare arena, The Pathologist points out. Their invention combines the smartphone’s native camera, an app, optomechanical lasers, and an algorithm contained within the attachment to carry out fluorescence microscopy in the field.
Future of Mobile-Testing
An article appearing in the Financial Times describes some of the ways mobile technology is changing healthcare, including diagnostics that have traditionally been performed in the medical pathology laboratories.
“Doctors scan your body to look for irregularities, but they rely on pathologists in the lab to accurately diagnose any infection,” the article notes. “There, body fluids such as blood, urine, or spit are tested for lurking microbes or unexpected metabolites or chemicals wreaking havoc in your body. Now companies are miniaturizing these tests to create mobile pathology labs.”
Apple introduced the first iPhone in 2007. It’s doubtful anyone imagined the innovations in diagnostics and pathology that would soon follow. Thus, trying to predict what may be coming in coming decades—or even next year—would be futile. However, scientists and researchers themselves are indicating the direction development is headed.
Should Essenlix and other mobile-lab-test developers succeed in their efforts, it would represent yet another tectonic shift for medical pathology laboratories. Clinical laboratory managers and stakeholders should be ready, for the words of the ancient Greek philosopher Heraclitus have never been truer: “Change is the only constant in life.”
—Dava Stewart
Related Information:
Mobile Phone Microscopy
How Smartphones Are Transforming Healthcare
This Startup Wants to Make Blood Testing as Easy as Snapping a Photo with an iPhone
Is mHealth an Opportunity or Threat to Medical Laboratories and Pathology Groups?
New FDA Regulations of Clinical Decision-Support/Digital Health Applications and Medical Software Has Consequences for Medical Laboratories
UCLA Device Enables Diagnosis of Antimicrobial Resistance in Any Setting; Could Save Lives Lost to Antimicrobial Resistant Bacteria
Lab-on-a-Chip Diagnostics: When Will Clinical Laboratories See the Revolution?
Tiny, Simple-to-Use Lensless Microscope Might Soon Find a Place in Pathology
Aug 31, 2018 | Digital Pathology, Laboratory Management and Operations, Laboratory News, Laboratory Operations, Laboratory Pathology, Laboratory Testing, Management & Operations
Affected patients speak about emotional, financial, and medical costs of receiving inaccurate results from the startup’s faulty Edison ‘finger-stick’ blood draw testing device
Healthcare consumers trust America’s clinical laboratories and anatomic pathology groups to provide accurate test results. When those test results are inaccurate, the loss of public trust can trigger a sharp decline in referrals/revenue and draw an avalanche of lawsuits by those harmed by inaccurate results.
The most recent example of this object lesson is disgraced blood testing company Theranos, previously estimated to be worth $9 billion but now struggling to stay afloat. The once high-flying startup has been brought to the edge of bankruptcy in the aftermath of a fraud settlement with the Securities and Exchange Commission (SEC), sanctions from the Centers for Medicare and Medicaid Services (CMS), investor lawsuits, consumer lawsuits, and a settlement with Walgreens over claims about Theranos’ Edison portable blood analyzer.
Theranos first made its unproven finger-stick blood draw device available to consumers in September 2013, when it announced a partnership with drugstore chain Walgreens (NASDAQ:WBA). At its height, Theranos operated 40 “Wellness Centers” in Walgreens stores in Arizona and a single location in California, which were the source of much of its revenue. USA Today reported the metro Phoenix-area centers alone sold more than 1.5 million blood tests, which yielded 7.8 million tests results for nearly 176,000 consumers. Theranos shuttered the wellness centers in 2016 after CMS inspectors found safety issues at Theranos’ laboratories in California and a Wall Street Journal (WSJ) investigation raised questions about the company’s testing procedures and accuracy claims. Ultimately, Theranos voided the results of all blood tests run on its Edison device from 2014 through 2015.

Breast-cancer survivor Sheri Ackert (above) told the WSJ she panicked when blood-test results from Theranos indicated her cancer may have reoccurred or were indicative of a rare type of tumor. After being retested by a different clinical laboratory, her results were found to be normal. Click here to watch a WSJ video about Ackert’s experience. (Photo/video copyright: Mark Peterman/Adya Beasley/Wall Street Journal.)
USA Today outlined the impact Theranos’ supposedly low-cost, cutting-edge technology had on several customers:
- A woman inaccurately diagnosed with the thyroid condition Hashimoto’s disease changed her lifestyle, made unnecessary medical appointments, and took medication she didn’t need;
- A woman inaccurately diagnosed with the autoimmune disease Sjögren’s syndrome was checked for food allergies before being retested and found not to have an autoimmune condition; and,
- An Arizona resident who had heart surgery visited a Theranos clinic five times to monitor the results of blood-thinning drug warfarin and was switched to a different drug. He had to have a second heart surgery to drain blood from the pericardial sac and believes more accurate test results could have averted the follow-up operation.
Arizona resident Steven Hammons visited a Theranos clinic several times to have his blood tested. He’d been placed on blood thinners following heart surgery. He was taken off the blood thinners presumably based on the results of those tests. However, as USA Today reported, one test result was later found to be inaccurate. Hammons, who underwent a second procedure to remove blood that had built up around his heart, told USA Today he was concerned about the safety of his fellow citizens.
“That makes me very concerned and worried for the safety of other Arizonans,” said Hammons, who once worked in the medical services division of a private health insurance company. “Government had a role in patient safety. The powers that be dropped the ball.”
Arizona Attorney General Mark Brnovich spearheaded a lawsuit against Theranos under the state’s Consumer Fraud Act, which led to a $4.65 million settlement covering full refunds for every Arizona customer who used the company’s testing services.
“Theranos may have not only had some erroneous test results, but they may have misread my rising blood pressure level as well,” Brnovich told The Republic in a 2017 article announcing the state’s fraud settlement with Theranos. “They said that about 10% of the results were inaccurate. The problem is, as an Arizona consumer, you don’t know whether you were part of that class or not.”
Downfall of a Once-Vaunted Clinical Laboratory Company
Dark Daily and sister publication The Dark Report have written extensively about these events. Former CEO Elizabeth Holmes founded Theranos in 2003 when she was just 19-years old. By 2013, Holmes had become a media sensation based on her claims that “Theranos had developed a medical technology that could do what seemed to be impossible: Its secret machines could run thousands of medical tests using the blood from a tiny finger-prick, and do so quickly and cheaply,” Bloomberg reported in a recent article outlining Holmes’ fall from grace.
While Holmes continues in the role of Chairman of Theranos’ Board of Directors, she was stripped of control of the company as part of the SEC settlement in 2016. The SEC found Holmes and then-company President Ramesh “Sunny” Balwani had fabricated claims Theranos technology had been validated by the Food and Drug Administration (FDA) and pharmaceutical companies and battle-tested by the US military in Afghanistan.
As a result, the SEC also barred Holmes from serving as an officer or director of any public company for 10 years. In October 2016, Theranos announced it would be closing its laboratory operations and focusing on its effort to create miniature medical testing machines, which it did. Nevertheless, the fallout continues.
As pressures on medical laboratories and pathology groups to cut costs while delivering quality care and value increases, laboratory leaders must not lose sight of the fact that accuracy of results remains the key to maintaining trust with healthcare consumers and a financially viable business.
—Andrea Downing Peck
Related Information:
Theranos, CEO Holmes, and Former President Balwani Charged with Massive Fraud
Theranos Receives Notice of Sanctions from the Centers for Medicare & Medicaid Services
Two More Investors Sue Theranos and Elizabeth Holmes for Fraud
Theranos Hit with Consumer Lawsuit over Faulty Blood Tests
Theranos, Walgreens Reportedly Reach a Deal to Settle Suit for under $30 Million
Theranos Selects Walgreens as a Long-Term Partner Through Which to Offer Its New Clinical Laboratory Service
An Open Letter from Elizabeth Holmes
How Startup Theranos Has Struggled with its Blood-Test Technology
Theranos Reaches $4.65 Million Fraud Settlement with Arizona
As Theranos Drama Unwinds, Former Patients Claim Inaccurate Tests Changed Their Lives
Theranos Statement on CMS 2567 Report
Agony, Alarm and Anger for People Hurt by Theranos’ Botched Blood Tests
Blood, Fraud and Money Led to Theranos CEO’s Fall from Grace
Holmes, Balwani Indicted by Department of Justice
Theranos News Gets Worse for the Former Silicon Valley Hero
After AACC Presentation, Elizabeth Holmes and Theranos Failed to Convince Clinical Laboratory Scientists and the News Media about Quality of Its Technology
Now Theranos Faces Criminal Investigation on Whether the Clinical Laboratory Company Misled Investors, according to Published Reports
Aug 23, 2018 | Digital Pathology, Laboratory Management and Operations, Laboratory News, Laboratory Operations, Laboratory Pathology, Laboratory Testing, Management & Operations
Genetic testing, gene sequencing done by clinical laboratories and anatomic pathology groups underpin how first-mover hospitals, health networks are improving patient outcomes
In just a few weeks, an unprecedented gathering will bring together the nation’s most prominent first-mover health networks, hospitals, and companies operating programs that deliver precision medicine daily to patients in clinical care settings.
On Sept. 12-13, 2018, “Breakthroughs with Genetic and Precision Medicine: What All Health Network CEOs Need to Know,” will take place at the Hutton Hotel in Nashville, Tenn. “What differentiates these sessions is the emphasis on each organization’s strategy, how it launched its precision medicine programs, what is improving in patient outcomes, and how payers are reimbursing for these services,” stated Robert L. Michel, Executive Director of the Precision Medicine Institute in Austin, Texas. “This is not about the science of precision medicine. Rather, it is about the practical elements required for any hospital, health system, or physician group to actually set up and deliver a precision medicine service to patients on a daily basis.”
Precision Medicine’s First-Mover Hospitals and Providers to Speak
Health systems and hospitals headlining this special conference are:
Companies scheduled to present include:
- Illumina;
- Humana;
- Sonic Healthcare USA;
- Genome Medical;
- CQuentia, and,
- S. HealthTek.
Exhibitors include the above, plus: Thermo Fisher, Philips, Sunquest, and MyGenetx.
“This meeting will give you the insider’s understanding about delivering precision medicine in real patient care settings that cannot be accessed at other venues,” noted Michel. “The goal is to have first-mover providers share their experiences, thus providing a road map that other hospitals, physician practices, and other providers at this conference can take back and follow with confidence.”
Michel said that sessions will be dedicated to precision medicine strategies, how it is being used in oncology, primary care, the role of pharmacogenomics, and use of healthcare big data. Speakers will describe the clever ways innovative health networks and hospitals are using healthcare big data to inform physicians in ways that improve outcomes, lower the cost of care and, in two real-world case studies, are generating seven-figure reimbursement from shared savings programs with certain health plans.

This year’s keynote address is by Jeffrey R. Balser, MD, PhD (above), President and CEO, Vanderbilt University Medical Center and Dean of the Vanderbilt University School of Medicine, one of the most progressive and innovative health systems in the country. (Photo copyright: Vanderbilt University.)
Using Healthcare Big Data to Achieve Precision Medicine Success, Shared Savings
“Shared savings successes will be one of the breakthrough achievements reported at the Nashville event,” he explained. “We’ve invited two prominent provider organizations to share how they are using healthcare big data to support physicians in achieving improved patient outcomes while at the same time impressively reducing the overall cost of care. To my knowledge, this is the first time these precision medicine case studies have been presented at a national meeting.”
One such presentation will be delivered by Philip Chen, MD, PhD, Chief Healthcare Informatics Officer at Sonic Healthcare USA Austin, Texas. Their precision medicine goal was to use healthcare big data to help physicians better manage diabetes and other chronic conditions in their practices. This program involved a large primary care practice and a major health insurer. Now in its fourth year, Sonic Healthcare USA is earning six- and seven-figure payments as part of a shared savings arrangement with the insurer.
“Shared savings is definitely a Holy Grail for all large health networks and physician groups as payers drop fee-for-service and switch providers to value-based payments,” said Michel. “The experience of Sonic Healthcare in this innovative three-way collaboration with an insurer and a very large physician group demonstrates that a strong data analytics capability and engagement with physicians can simultaneously bend the cost-of-care-curve downward while improving patient outcomes, as measured year-by-year. This is a presentation every C-Suite executive should attend.
Strategic, Business, Operational, and Financial Aspects of Precision Medicine
“This conference—centered upon the strategic, business, operational, and financial aspects of a precision medicine program—came to be because it is the unmet need of every health network CEO and C-Suite administrator,” observed Michel. “Every healthcare leader tasked with developing an effective clinical and financial strategy for his or her institution knows that the real challenge in launching a precision medicine program for patient care is not the science.
“Rather, the true challenges come from how to support clinical needs with the availability of capital, recruiting experienced clinicians, and putting the right informatics capabilities in place,” he stated. “Most hospital and health network administrators recognize the risk of launching a precision medicine program too early. They know such programs can suck up huge amounts of resources without producing significant improvements in patient care. What adds to the risk is that payers may be slow to reimburse for precision medicine.”
Register today to guarantee your place at “Breakthroughs with Genetic and Precision Medicine: What All Health Network CEOs Need to Know,” (or copy and paste this URL in your browser: https://dark.regfox.com/precision-medicine-institute).
Register by September 1 and save $300 on tuition! Plus, take advantage of our special Team Discount Program, so you and your key team members can get the most out of the conference by attending together.
“Breakthroughs with Genetic and Precision Medicine: What All Health Network CEOs Need to Know” is the gold-standard summit for everyone active or interested in succeeding with precision medicine programs. Don’t miss out—register today!
—Michael McBride
Related Information:
Breakthroughs with Genetic and Precision Medicine: What All Health Network CEOs Need to Know—Full Agenda and Details
Breakthroughs with Genetic and Precision Medicine: What All Health Network CEOs Need to Know—Registration information
Ongoing Growth in Consumer Genetic Testing Pressures Hospitals, Healthcare Networks to Educate and Prepare Physicians
Syapse Creates Precision Medicine Council That Quickly Attracted 200 of the Biggest Hospitals and Health Networks as Members
When Ramping Up Genomic Programs, Health Network/Hospital CEOs and Executives Must Consider Emerging Technologies, Swiftly Rising Consumer Demand
Precision Medicine Success Hinges on Diagnostics’ Clinical Utility
Precision Medicine and Sharing Medical Data in Real Time: Opportunities and Barriers
Ongoing Growth in Volume of Clinical Laboratory Tests That Support Precision Medicine Due to Physician Acceptance; Payers Still Have Concerns
Aug 17, 2018 | Digital Pathology, Laboratory News, Laboratory Operations, Laboratory Pathology, Laboratory Testing, Management & Operations
Pathologists might be able to help overburdened doctors by adding medical laboratory support services that assist providers in selecting the right tests and identifying the best therapeutic options for patients
In a new Stanford University School of Medicine study published in the July 9, 2018, issue of Mayo Clinic Proceedings, researchers indicate that physician burnout may be as big a cause of medical errors as unsafe healthcare environments. This highlights an opportunity for clinical laboratory professionals and pathologists to help physicians improve both diagnostic accuracy and the selection of the most appropriate therapies.
The study found that exhausted providers were twice as likely to report making a medical error. However, it’s a complex problem with no easy solutions.
“Just trying to fix the setting of healthcare environments in order to prevent errors is not sufficient,” Stanford University’s Daniel Tawfik, MD, MS, the study’s lead author, told Reuters Health. “We also need to address the actual underlying human factors that contribute to errors—specifically looking at physician burnout.”
Nevertheless, while there is no one-size-fits-all solution to physician burnout, clinical laboratory managers and pathologists potentially could help overburdened providers reduce burnout and fatigue by adopting new lab testing support services designed to assist physicians in selecting the right tests and identifying the best therapeutic options for their patients.
Medical Errors Third-Leading Cause of Death in America
Stanford researchers wanted to learn how physician burnout contributes to medical errors which, according to Johns Hopkins, is the third-leading cause of death in the US. They surveyed 6,695 physicians from across America. Of the respondents:
- More than 54% reported symptoms of burnout;
- 33% experienced excessive fatigue;
- Nearly 7% had thoughts of suicide; and,
- Roughly 4% reported a failing safety grade in their primary work area.
Even in medical units judged to have excellent safety records, the study found rates of medical errors nearly tripled when physicians working in those units had high levels of burnout. The prevalence of errors became similar to a non-burned-out physician working in a unit with a safety grade of “acceptable” or “poor.”
“We found that physicians with burnout had more than twice the odds of self-reported medical error, after adjusting for specialty, work hours, fatigue, and work unit safety rating,” Tawfik noted in a Stanford news release. “We also found that low safety grades in work units were associated with three to four times the odds of medical errors.”
According to the study, overall, 10.5% of physicians surveyed acknowledged in the prior three months making:
- An error in judgment;
- A wrong diagnosis;
- A technical mistake during a procedure;
- Prescribing a wrong drug/dosage; and/or,
- Ordering medication/intervention for the wrong patient.
While more than half of mistakes (55.4%) did not affect patient outcomes, or only caused a temporary problem (22.6%), more than 5% of errors did lead to major permanent health problems and 4.5% resulted in a patient death, the study found.
Radiologists, neurosurgeons, and emergency medicine specialists had the highest prevalence of error rates, with more than 21% of providers in each of those fields acknowledging recent mistakes.
Physicians reporting errors were more likely to have symptoms of overall burnout (77.6% versus 51.5%), as well as fatigue (46.6% versus 31.2%), than error-free providers. Physicians reporting recent errors also had a higher prevalence of suicidal thoughts (12.7% versus 5.8%), the study found.
Ted Hole, MD, a family practice physician in Ventura, Calif., is not surprised by the correlation between medical mistakes and overall well-being. “If your brain isn’t working right, you’re going to make errors,” Hole told the Ventura County Star. “That’s what burnout does. It makes your brain not work right.”
Stanford Connects Physician Burnout and Poor Workspace Safety Ratings
In their paper, the Stanford researchers argue a “combination of physician-targeted burnout interventions and unit-targeted patient improvement measures” are needed to tackle the problem of medical errors. Physicians who gave their work units an excellent, very good, or acceptable safety grade were less likely to make a medical error than those who described workplace safety as poor or failing.
Of the physicians who reported a poor or failing work unit safety grade, nearly 25% reported a recent error. Errors were incrementally lower for work units with higher safety grades regardless of physician burnout levels.
“This indicates both the burnout level as well as work unit safety characteristics are independently related to the risk of errors,” Tait Shanafelt, MD, Director of the Stanford WellMD Center and Associate Dean of the School of Medicine, noted in a Stanford statement.
“Today, most organizations invest substantial resources and have a system-level approach to improve safety on every work unit,” he said in the Stanford news release. “We need a holistic and systems-based approach to address the epidemic of burnout among healthcare providers if we are truly going to create the high-quality healthcare system we aspire to.”

Tait Shanafelt, MD (above), is Director of the Stanford WellMD Center, Associate Dean of the School of Medicine, and an author of the Stanford study. He maintains the “epidemic of burnout” among healthcare providers should receive as much attention as safety issues. Shanafelt became Stanford Medicine’s first Chief Wellness Officer in 2017. (Photo copyright: Stanford School of Medicine.)
Burnout Among Physicians Increasing
Other studies, including Medscape’s “Lifestyle Report 2017: Race and Ethnicity, Bias and Burnout,” confirm an upward trend in burnout rates among US physicians. In the Medscape study, 51% of physicians surveyed reporting being “burned out,” defined as a loss of enthusiasm for work, feelings of cynicism, and a low sense of personal accomplishment. Since the Medscape Lifestyle Report first queried physicians about burnout in 2013, the number of providers reporting burnout has increased 25%.
Physician burnout has been attributed to a variety of factors, including:
- Excessive workloads;
- Financial stress;
- Extra hours spent on clerical work or EHR-related tasks; and,
- Loss of human-to-human interaction between physician and patient.
Robert Lum, MD, an Oxnard, Calif.-based radiation oncologist, blames the shift to corporate-owned medical practices for some of the reported increases in burnout among physicians. Lum told the Ventura County Star he stays upbeat by never losing sight of why he became a physician.
“If you focus on the reason you went into medicine in the first place, which is to help people and marvel at the miracles modern medicine is able to do, then you’ll have less burnout,” he said.
Nevertheless, other solutions also can help. Clinical laboratories play a key role in maximizing physician/patient encounters. By extension, physicians and laboratories are linked in unique ways that enable labs to reduce physician burden and ensure positive healthcare outcomes.
—Andrea Downing Peck
Related Information:
Physician Burnout, Well-being, and Work Unit Safety Grades in Relationship to Reported Medical Errors
Study Suggests Medical Errors Now the Third Leading Cause of Death in the U.S.
Medical Errors May Stem more from Physician Burnout than Unsafe Health Care Settings
Study Says Rising Doctor Burnout Means Rising Medical Errors
In a First for U.S. Academic Medical Center, Stanford Medicine Hires Chief Physician Wellness Officer
Medscape Lifestyle Report 2017: Race and Ethnicity, Bias and Burnout
Physician Burnout a Key Driver of Medical Errors
Aug 15, 2018 | Digital Pathology, Laboratory Management and Operations, Laboratory News, Laboratory Operations, Laboratory Pathology, Laboratory Testing
Using precision genomics, Mayo researchers hope to develop improved medical laboratory tools for screening, diagnosing, and treating patients with inherited genetic disorders such as accelerated aging
Telomeres increasingly are on the radars of physicians and healthcare consumers alike, as researchers gain more knowledge about these critical nucleotides, and doctors continue to indicate their belief that telomeres could make useful diagnostic tools. If so, that would open up a new channel of precision medicine testing for clinical laboratories and anatomic pathology groups.
Telomeres are DNA strands that protect chromosome end points from degrading as people age. Their job is similar to the way plastic tips keep shoelaces from fraying, researchers at the Mayo Clinic explained in a news release. They have been using precision genomics in their assessment of 17 patients with short telomere syndrome (STS) to uncover the genetic causes of the condition.
They published their findings in the July issue of Mayo Clinic Proceedings.
Using Genetic Sequencing to Find Causes of Short Telomeres
People with STS could develop conditions including bone marrow failure, liver disease, and lung disease earlier in life than others, the news release pointed out.
However, according to the researchers’ paper, “Management of STSs is fraught with significant challenges such as delayed diagnoses, lack of routinely available diagnostics modalities, and standardized treatment guidelines.”
Nevertheless, some physicians are already leveraging information about telomeres in patient treatment. And many consumers have been turning to telomere diagnostic testing companies to learn the lengths of their own telomeres. They’ve learned that the longer the telomeres the better, as shorter telomeres are associated with accelerated aging.

“The length of certain telomeres gives a history of all the assaults a person has been subject to over the course of her lifetime,” a Wired article noted, quoting Joseph Raffaele, MD, co-founder of PhysioAge Medical Group, a clinical practice in New York City that specializes in “proactive” medicines. He goes on to call telomeres “the new cholesterol.” (Photo copyright: drraffaele.com.)
More Study into STS is Needed
GenomeWeb summarized the Mayo study’s methodology as follows:
Researchers reported these findings in Mayo Clinic Proceedings:
Study authors concluded that while some genetic mutations are common to short telomeres, they were found in only about 40% of the people in their study. So, more research is needed to discover other causes of short telomeres.
Telomeres and Lung Disease
Other research into telomeres was conducted by St. Paul’s Hospital and the University of British Columbia Department of Medicine, which focused on telomeres and lung disease.
In this study, researchers used polymerase chain reaction (PCR) to measure absolute telomere length from blood samples provided by 576 people with chronic obstructive pulmonary disease (COPD), according to a paper in the journal CHEST, published by the American College of Chest Physicians.
The study found that when compared to people with normal blood telomeres, people with shorter telomere lengths and more rapidly aging blood cells:
- Were 50% more likely to develop new or increasing respiratory symptoms;
- Were nine times more likely to die; and,
- Had worse health status and quality of life.
“It is known that short telomeres are associated with common morbidities of COPD, but it was not known if there is a relationship between blood telomeres and patient-related outcomes in COPD,” Don Sin, MD, a chest physician who led the research at the Centre for Heart Lung Innovation at St. Paul’s Hospital, stated in a news release.
Other Takes on Telomeres
A Harvard Medical blog noted, however, that short telomeres do not necessarily mean disease is imminent, nor that long ones guarantee optimal health.
“There is mounting evidence that a healthy lifestyle buffers your telomeres,” stated Immaculata De Vivo, PhD, a Harvard Medical School Professor and Genetics Researcher at the Dana-Farber/Harvard Cancer Center, in the blog post.
However, another expert questions the value of measuring telomeres for disease risk.
“In short, telomere lengths are too variable within a population, too variable within an individual, and too sensitive to environmental factors to offer any reliable information for common disease risk,” wrote Ricki Lewis, PhD, in PLOS.
Although there are many pitfalls to overcome, some doctors are pushing to use telomere information in patient treatment, and these studies from the Mayo Clinic and other researchers have contributed important data for diagnostic test developers.
In the end, vast and varied content about telomeres exists and clinical laboratory professionals may be called on to help clarify and assess the information. And that’s the long and the short of it.
—Donna Marie Pocius
Related Information:
Precision Genomics Point the Way to Mutations Associated with Accelerated Aging
Telomeres Are the New Cholesterol. Now What?
Clinical Correlates and Treatment Outcomes for Patients with Short Telomeres Syndrome
Mayo Clinic Researchers Use Targeted Sequencing to Diagnose Short Telomere Syndrome
Relationship of Absolute Telomere Length with Quality of Life, Exacerbations, and Mortality in COPD
Blood Telomeres Can Help Predict Risk of Disease Worsening or Death in COPD Patients
Can DNA Markers Called Telomeres Predict Aging?
Telomere Testing: Science or Snake Oil?
White Paper Download | How Next-Generation Sequencing Helps Molecular Laboratories Deliver Personalized Medicine Services to their Client Physicians
Summit: Breakthroughs with Genetic and Precision Medicine: What All Health Network CEOs Need to Know











